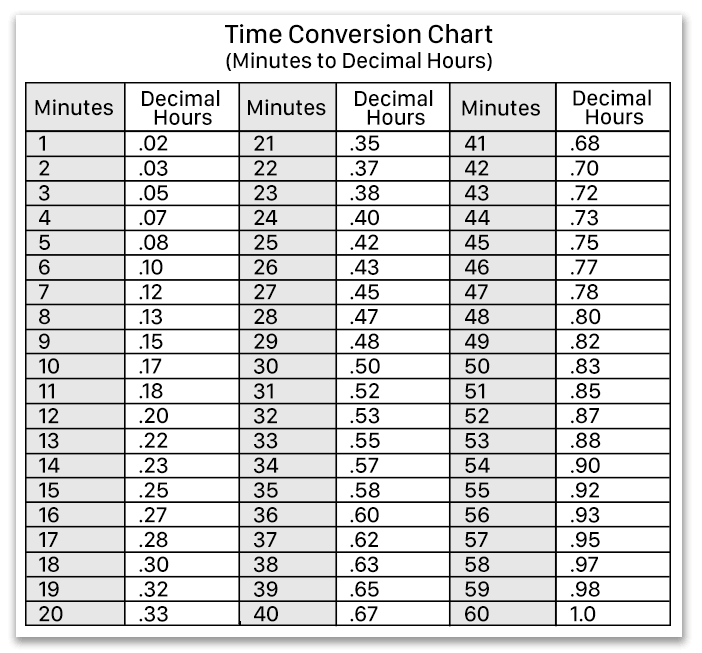
Then, check your total against the chart below to see the maximum total number of codes you can bill: So, to figure out how many total billing units you have, you should always start by adding up your one-on-one time (leave unattended time out of the equation). However, when untimed codes come into play, things get a little more confusing. To give a simple example, if you performed manual therapy for 15 minutes and ultrasound for 8 minutes, you could bill two direct time units. But if seven or fewer minutes remain, Medicare will not reimburse you for another full unit, and you must essentially drop the remainder. If eight or more minutes are left over, you can bill for an additional unit. 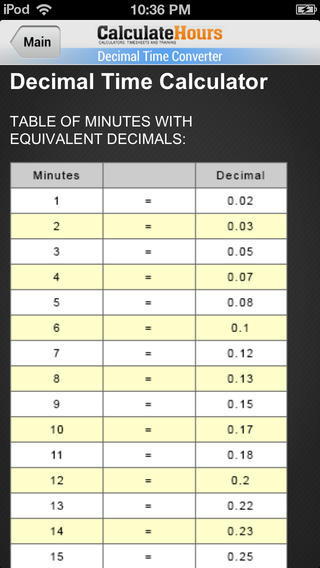
In other words, Medicare adds up the total minutes of skilled, one-on-one therapy (direct time) and divides the resulting sum by 15. What if you only provide ultrasound for 11 minutes? Or manual therapy for 6 minutes? That’s where the 8-Minute Rule comes in: Per Medicare rules, in order to bill one unit of a timed CPT code, you must perform the associated modality for at least 8 minutes. But your treatment time for these codes won’t always divide into perfect 15-minute blocks. 
Minutes and Billing UnitsĪccording to CPT guidelines, each timed code represents 15 minutes of treatment. These are the codes you use for one-on-one, constant attendance procedures and modalities such as therapeutic exercise or activities, manual therapy, neuromuscular re-education, gait training, ultrasound, iontophoresis, or electrical stimulation (attended). Time-based (or direct time) codes, on the other hand, allow you to bill multiple units in 15-minute increments (i.e., one unit = 15 minutes of direct therapy). For services like these, you can’t bill more than one unit-regardless of the amount of time you spend delivering treatment. You would use a service-based (or untimed) code to denote services such as conducting a physical therapy examination or re-examination, applying hot or cold packs, or providing electrical stimulation (unattended). So first, let’s talk about the difference between time-based and service-based CPT codes. It might sound simple enough, but things get a little hairy when you bill both time-based and service-based codes for a single patient visit. (This rule also applies to other insurances that have specified they follow Medicare billing guidelines.) Basically, a therapist must provide direct, one-on-one therapy for at least eight minutes to receive reimbursement for one unit of a time-based treatment code. The 8-Minute Rule governs the process by which rehab therapists determine how many units they should bill to Medicare for the outpatient therapy services they provide on a particular date of service. So, here’s a rundown of the rule-and a short explanation of how it works in WebPT. Yes, I’m talking about the dreaded 8-Minute Rule (a.k.a. When it comes to Medicare units and payment for physical therapy services, however, things aren’t always so simple. There are no complicated formulas for determining the monetary value of a pizza or a movie ticket you simply pay the business’s advertised price. With most buyer-seller transactions, calculating the cost of a product or service is fairly simple.
0 Comments
Leave a Reply. |
 RSS Feed
RSS Feed
